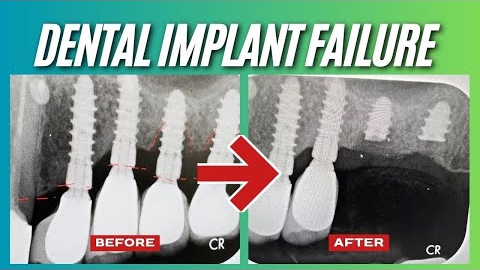
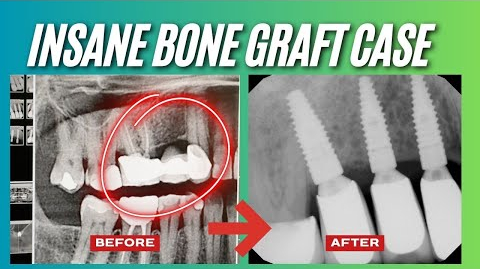
Dental implants are designed to last, but they still rely on healthy bone and gum tissue for long-term success. When bone loss develops around an implant, it can put the entire restoration at risk.
For many patients in Poway, CA, this type of issue can go unnoticed at first. You might see minor bleeding when brushing, some tenderness, or changes on an X-ray, but before anything feels serious. The good news is that when caught early, treatment can often help preserve the implant and prevent more complex procedures.
Watch: See how gum grafting can help protect dental implants affected by bone loss.
What Bone Loss Around a Dental Implant Really Means
Bone loss around an implant is usually a sign of inflammation in the surrounding tissue. Over time, this inflammation can break down the bone that supports the implant, making it harder to clean and maintain.
Unlike natural teeth, dental implants don’t have the same blood supply. That difference makes healing and regeneration more limited in certain situations—especially when bone loss occurs in tight spaces around the implant.
This is why early intervention matters. Once the environment around the implant becomes difficult to maintain, the problem tends to progress.
Why Bone Grafting Isn’t Always the Best Solution
When people hear “bone loss,” the first assumption is often that bone grafting is the answer.
In some cases, that’s true. Procedures like bone grafting for dental implants are highly effective when rebuilding bone in open areas. But around dental implants—especially in narrow or confined spaces, bone regeneration is often not predictable or effective.
That’s because:
- Implants are made of titanium and don’t behave like natural teeth
- Blood supply in tight spaces is limited
- The environment may not support stable bone regrowth
In these situations, trying to rebuild bone alone doesn’t always solve the problem.
A Better Approach: Strengthening the Gum Tissue
Instead of focusing only on rebuilding bone, treatment often shifts to improving the soft tissue around the implant.
This is where gum grafting becomes a powerful solution.
Building up a thicker gingiva (Keratinized Tissue ) around the implant, patients often experience:
- Less discomfort when brushing
- Easier hygiene
- Reduced inflammation
- And the MOST important: Preserving the remaining of the bone around the implant to avoid Peri-Implantitis gum infections on dental implants
This approach is often more predictable and practical than attempting bone regeneration in a compromised area.
What Is “Biotype Conversion” and Why It Matters
One of the most important concepts in this type of treatment is something called biotype conversion.
Some patients naturally have thin, fragile gum tissue. Around implants, this can make the area sensitive, difficult to clean, and more prone to inflammation.
Gum grafting changes that.
It transforms thin tissue into thicker, more durable tissue that is easier to maintain and more resistant to irritation. Over time, this improved environment helps stabilize the implant and reduce the risk of further bone loss.
How Gum Grafting Around an Implant Works
Gum grafting is a precise procedure designed to strengthen the tissue around an implant.
A small amount of tissue is typically taken from the roof of the mouth and placed in the area where additional support is needed. The site is carefully prepared to ensure a strong blood supply so the graft can heal and integrate properly.
As the tissue heals, it becomes thicker and more resilient. For many patients, this leads to noticeable improvements in comfort and daily oral hygiene.
If you want to better understand how implants are maintained long-term, visit the dental implants page.
Why Thick Gum Tissue Makes a Big Difference
Thin tissue often creates a cycle:
Brushing feels uncomfortable → the area gets avoided → plaque builds up → inflammation worsens.
Thicker tissue breaks that cycle.
It creates a more stable, comfortable environment that makes brushing easier and helps keep bacteria under control. Over time, this plays a major role in protecting the implant.
Ongoing care, including periodontal maintenance, is also key to keeping implants healthy after treatment.
When to Have a Dental Implant Evaluated
Bone loss around implants isn’t always obvious early on. Some patients only discover it during routine imaging, while others notice symptoms sooner.
Common signs include:
- Bleeding around the implant
- Tenderness when brushing
- Gum recession
- Food trapping in the area
If you’re experiencing any of these, it’s worth having the implant evaluated before the condition progresses.
Dental Implant Treatment in Poway, CA
For patients in Poway and nearby areas like Rancho Bernardo, Scripps Ranch, and Escondido, treating implant complications early can make a significant difference.
At Poway Perio, treatment focuses on identifying the cause of bone loss and improving both the bone and soft tissue environment around the implant. By combining advanced imaging with personalized care, many patients can stabilize their implants and avoid more invasive procedures.
If you’re concerned about an implant or noticing early signs of bone loss, you can schedule a consultation to explore your options.
FAQs: Bone Loss Around Dental Implants
Can bone loss around dental implants be reversed?
Bone loss can sometimes be improved, but most treatment focuses on stopping progression and protecting the remaining bone through procedures like gum grafting.
What is peri-implantitis?
Peri-implantitis is an inflammatory condition that affects the gum and bone around implants. Learn more about related issues like gum infections on dental implants.
Is gum grafting painful?
Most patients experience minimal discomfort, especially with modern techniques. Recovery is typically manageable and improves quickly within the first week. You can also review healing after gum grafting tips for recovery to better understand the process.
How long does gum grafting take to heal?
Initial healing usually takes 1–2 weeks, with full integration over several weeks. For a detailed timeline, see healing after gum grafting tips for recovery.
Can gum grafting save a failing dental implant?
In many cases, yes. By improving tissue thickness and reducing inflammation, gum grafting helps stabilize the implant and protect remaining bone.
When is bone grafting needed for dental implants?
Bone grafting is typically used when there is significant bone loss or when preparing for implant placement. Learn more about bone grafting for dental implants.
What are the early signs of dental implant failure?
Bleeding, swelling, discomfort, gum recession, and difficulty cleaning the area are common early warning signs. Ongoing care, like periodontal maintenance, can help catch these issues early.
How can I prevent bone loss around my implant?
Consistent oral hygiene and professional cleanings are key. Regular visits for periodontal maintenance help prevent inflammation and long-term complications.
Is gum grafting only for receding gums?
No. While it’s commonly used for recession, gum grafting is also highly effective for strengthening tissue around dental implants.
Who should I see for implant-related gum issues in Poway?
A periodontist specializes in gum and implant health. You can schedule a consultation or contact Poway Perio to have your implant evaluated.